
The skin is the largest organ in your body. It is also the most visible one and is often referred to as the window into a person’s overall well-being. The skin carries a clue about the health of other organs. Changes in the skin color or texture may sometimes indicate severe health conditions, according to dermatologists.
Drug and alcohol use can have severe consequences on the body organs. Drugs like cocaine, and heroin can significantly stress the heart and damage kidneys. Alcohol, on the other hand, puts tremendous strain on the liver. But since it is impossible to see what’s happening in the body with bare eyes, the damage may go unnoticed for years.
Luckily, you can identify drug or alcohol-related issues by looking at the skin. When drug users abuse substances for a long time, they may experience sores, inflammation, infections, lesions, and even skin rotting. This happens for a range of reasons, including:

Regular skin problems can be a sign of drug abuse.
Substance abuse can cause dehydration through the effects of the drugs themselves. Illegal drugs are known to increase sweating, speed of breathing, urination, and diarrhea, and vomiting. In some cases, the drugs make a person over-active, interfering with the body’s awareness and attention to ignore the need for fluid. Dehydration is characterized by dry eyes, chapped lips, dry mouth, and feeling thirsty. Prolonged use may also cause dry, flaky skin. Dry skin is more prone to wounds, blemishes, and poor healing.
Rashes are common in heavy meth users. They manifest as festering and painful-looking sores. Meth (and cocaine) users develop sores for various reasons, but the most common is that they pick and scratch their skin. They do so because it feels as though bugs are burrowing underneath the skin. Some say they feel a sensation of drug coming out of their skin. So they pick at it to the extent that they tear their flesh open. Meth mites – the feeling that insects or bugs are crawling under or on the skin – is a common side effect of excessive methamphetamine use. It’s also the biggest giveaway of meth addiction.
Heroin use may also lead to intense itching because it triggers the production of histamine. It may cause immense, blistering rash or dark patch on the skin (with velvety feel). Heroin use may also cause red patches to form all over the body.

Healthy skin can deteriorate at a rapid pace when illicit drugs are being used.
Another reason meth users develop sores is that the drug isn’t clean. It’s made with battery acid, which causes abscesses. And the byproducts used during its production can irritate the skin and cause itchy red sores that look like burning skin rash. Besides, crystal meth suppresses the immune system, making it hard for the body to fight off infections and bacteria. Couple that with poor hygiene, and you create a perfect storm for meth rash. This can occur in the face, arm, shoulder, back, and between the legs.
Some drug dealers add other substances to cocaine to stretch their product and increase profit margins. One such substance is levamisole, which is linked to necrotizing fasciitis, a skin-eating disease. It manifests in an extreme blackening of the outer ear and reddening of the cheeks. The same effects may happen on the back, chest, buttocks, legs, and abdomen.
Not everyone who uses drugs will experience skin disorders. It’s all up to a person’s genetic markup. Stimulants can cause hypersensitivity, hives, cold sores, and the swelling of the epidermis. In extreme cases, these drugs can cause severe conditions like Toxic Epidermal Necrolysis (TEN) and Stevens - Johnson syndrome (SJS).
SJS is a rare yet severe skin and mucous membranes. It is characterized by a painful rash that blisters and spreads. The outer layer of the rash dies, peels off and starts to heal after several days. A more severe form of SJS is called TEN. TEN is a rare and potentially life-threatening condition that affects over 30% of the skin and causes immense damage to the mucous membranes. In TEN, the peeling progresses fast, leading to large raw areas that may weep or ooze.
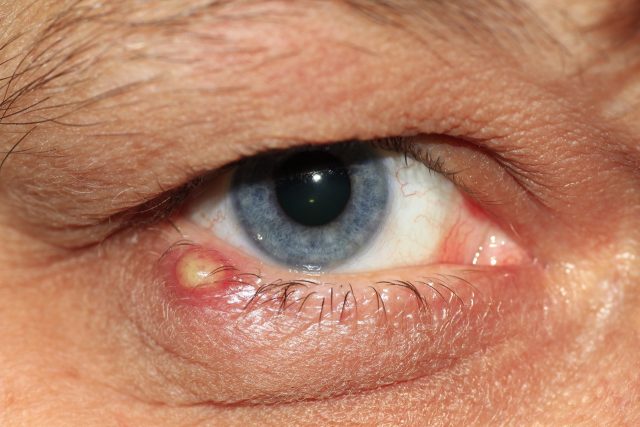
Unexplained sores, rashes and scabs are common with certain types of drugs.
According to the American Academy of Dermatology, atopic dermatitis (AD) is a common skin condition that affects more than 1 in 10 Americans. However, the condition, which makes the skin red and itchy, is common among those struggling with drug addiction. AD is a chronic pruritic inflammatory skin condition that mostly affects the neck, arms, cheeks, and legs.
These usually arise because of smoke, weight loss, or other toxins. But drug use can also cause premature aging, lines, wrinkles, and so on. Smoking drugs like heroin, crack, cocaine, meth, or marijuana harms the skin, creating a wrinkled, leather-like texture that makes one look older. Smoking also speeds up and facilitates skin conditions like eczema, psoriasis, and even skin cancer.
When a drug-dependent person is dehydrated, exhausted and malnourished, they may experience drug-induced hyperpigmentation. This is where they experience color changes in the skin, folds, and spots in different parts of the body. Drugs like heroin, prescription meds, crack cocaine, and cocaine can cause a nutritional problem. Advanced stages of addiction can make one neglect regular foods and meals, leading to exhaustion and malnutrition.
Since the drugs lower the body’s immunity, any infection that shows up in the skin may take a long time to heal. Sometimes, it might worsen. Many cocaine and heroin users who inject drugs develop infections at the injection point, which becomes severe with repeated use.

The sooner you address a problem with drugs or alcohol, the easier it will be to treat. Get help now, before it's too late!
Treatment programs exist to help those struggling with drug addiction to overcome their using problem, and resulting skin problems. Addiction treatment allows patients to heal their mind, body, and spirit. Most of these centers have experts who can offer medical advice, diagnosis, or treatment. In extreme cases, these experts may refer the patient to a specialist.